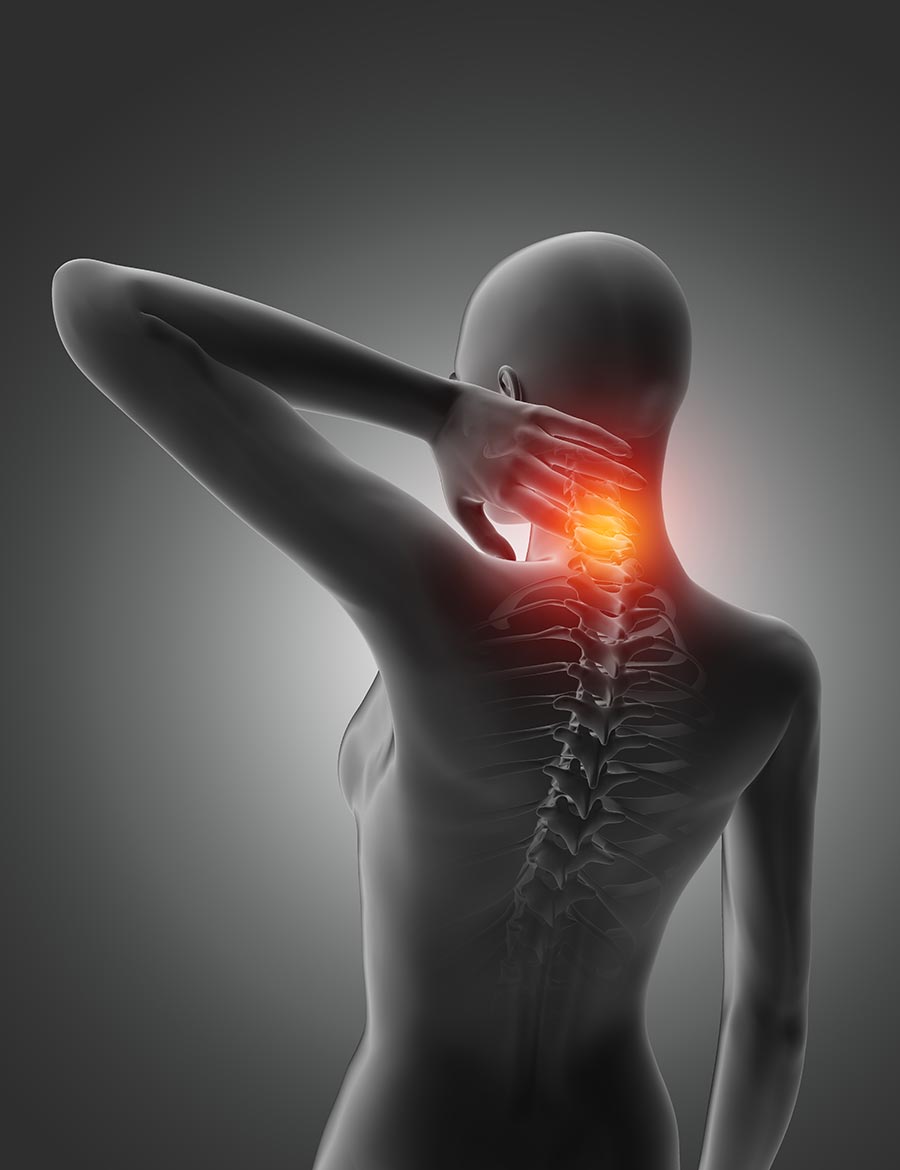
Cervical Spondylosis
![]()
Call (703) 520-1031 or use the form to send us your contacts.
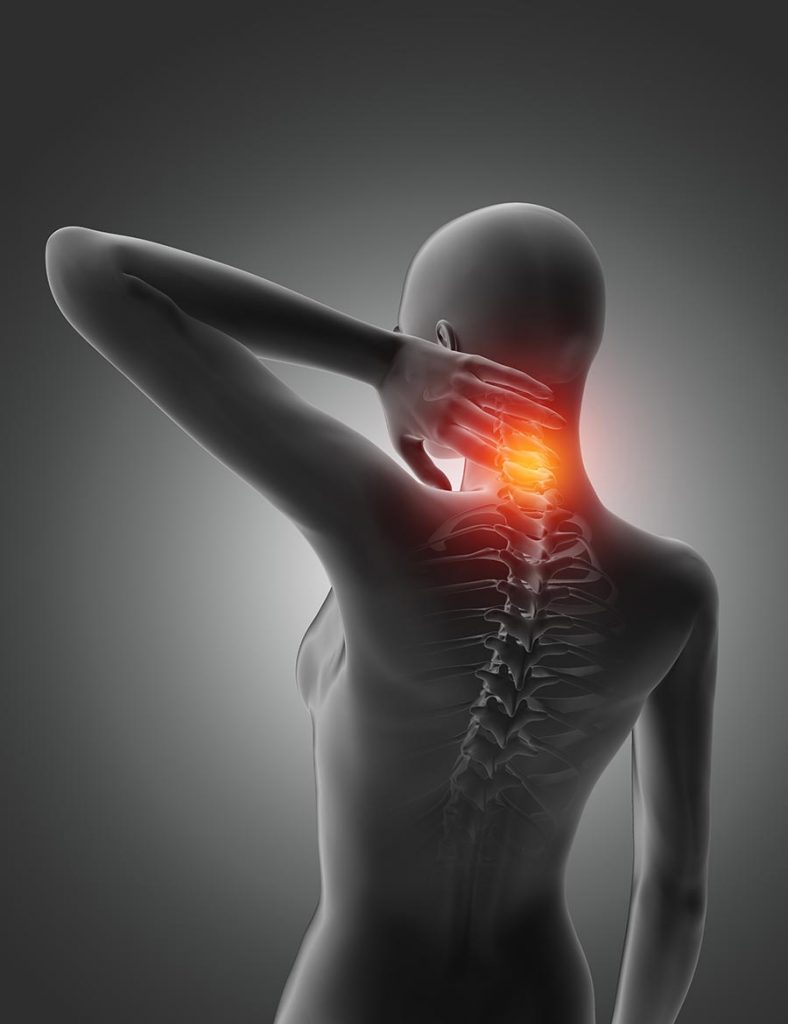
What is Cervical Spondylosis?
Cervical spondylosis is the name for a general medical condition in which the spinal discs in the neck (cervical spine) experience wear and tear for some reason. The discs that serve as cushions between the spine’s bones become dehydrated, causing them to shrink or become compressed. The changes to the discs lead to other anatomical changes in the supporting structures in the neck, like joints and ligaments. Conditions like osteoarthritis and bone spurs can develop as a result.
Cervical Spondylosis Causes
Cervical spondylosis is a degenerative disease affecting millions of people. Research has shown that it is detectable in a majority of people who are over 50 years old. The most common trigger for developing the degenerative condition is normal wear-and-tear due to aging. The degeneration process usually starts during the middle-age years.
Cervical spondylosis, a general term, is caused by the following specific conditions or changes in the cervical spine.
Degeneration of cervical spine discs
The spinal discs are thin and lose elasticity. As discs deteriorate and collapse, the vertebrae above and below the discs get closer together. The change in vertebral alignment causes the facet joints to touch. This can lead to bone spurs’ development, which can grow into the spinal canal and pinch the spinal cord and nerves (spinal stenosis).
Herniation
A herniated disc is one that has torn or cracked and can rupture or break open. This allows the nucleus pulposus (disc nucleus) to ooze out through the tear, pinching the spinal cord and nerves. When the herniated disc places pressure on a spinal nerve or surrounding tissue, pain, numbness, or weakness can occur.
Bulging disc
A cervical disc may slip out of place (slipped disc) or bulge out. A spondylotic protrusion is a disc that pouches out when it degenerates and weakens, usually due to normal aging. The disc itself remains intact, though. The bulging disc may or may not compress nerves.
Osteoarthritis
When the cartilage cushioning the bone ends deteriorates, osteoarthritis develops. Spinal joints become painful, swollen, or stiff, and the range of neck motion might be limited. If the cartilage thins enough, the bone starts rubbing against it. This can lead to osteophytes or bone spurs, abnormal bone growths.
Bone spurs
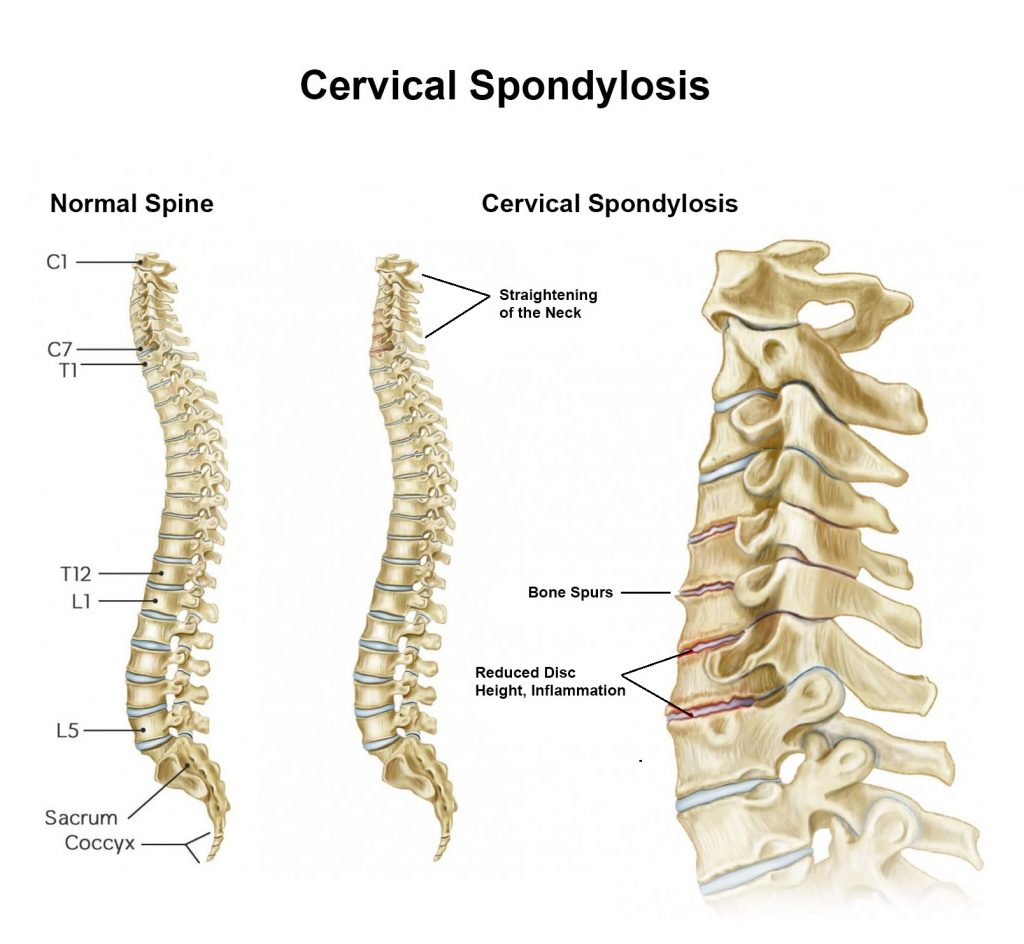
Cervical Spondylosis Symptoms
One of the interesting facts about cervical spondylosis is that there may not be any symptoms indicating the condition has developed. It depends on how the shrinking or compressing disc impacts the space in the spine where the spinal cord and nerve roots pass. If the spinal cord is compressed, cervical nerves might be pinched.
Osteophytes are bone spurs that are a typical result of aging. Spurs develop due to new bone cells being deposited during the bone renewal process in places where they would not normally grow. They often accompany conditions like degenerative disc disease, spinal stenosis, and osteoarthritis. They do not produce symptoms in many people, but it depends on how they grow.
Cervical spondylosis symptoms vary from person to person, but the common symptoms are the following.
- Neck pain
- Inflammation
- Headaches
- Neck stiffness
- Numbness or tingling in the shoulders, arms, hands, legs or feet
- Weakness in the arms, hands, legs or feet
- A feeling of grinding when moving the neck
- Difficulty walking
- Lack of coordination or trouble maintaining balance
- Loss of bowel or bladder control
It is essential to see a doctor immediately if there is a sudden issue with numbness or weakness in various areas of the body or difficulty with or loss of bowel or bladder control.
Who is at Risk of Developing Cervical Spondylosis?
The people at most risk of developing cervical spondylosis include the following.
- People over the age of 60
- Prior injury to the neck
- Jobs that require repetitive neck motions or any positions that put additional stress on the neck, like repeated lifting or reaching overhead
- Genetic factors appear to play a role when there is a family history of spondylosis (medical research is ongoing)
- Poor posture leading to spinal changes
- Being overweight or obese due to extra stress placed on the joints
- Past spine surgery
Smoking has also been connected to the worsening of degenerative disc disease in the cervical spine. Research presented to the Association of Academic Physiatrists demonstrated smoking negatively impacts blood vessels in a way that impedes the nourishment of intervertebral discs.
How do Healthcare Providers Diagnose Cervical Spondylosis?
A doctor will diagnose spondylosis of the cervical spine by conducting a physical exam and ordering one or more medical tests. The physical exam will include checking the neck’s range of motion, watching how you walk, and testing reflexes to determine if pressure on the spinal nerves or the spinal cord impacts muscle strength. It is essential to tell the doctor all the symptoms experienced, including the location of any numbness and weakness, and pain.
There are various imaging and nerve function diagnostics tests the doctor can choose from based on the physical exam results.
Imaging tests include:
- X-rays detect abnormalities in joints and bones in the neck, like bone spurs
- MRI detects pinched nerves
- CT scan delivers detailed imaging of bones and soft tissues
- Myelography – tracer dye injected into the spinal canal provides more detail for imaging tests
Nerve function tests include:
- Nerve conduction study – electrodes placed on the skin send small shocks to nerves to enable measuring nerve response
- Electromyography – measures nerve electrical activity while the nerves are transmitting signals to the muscles when the muscles are resting and contracting
Treatment
The severity of the symptoms and condition determines the treatment for cervical spine spondylosis. For mild cervical spondylosis pain or discomfort, most people first try over-the-counter pain relievers, such as NSAIDs (nonsteroidal anti-inflammatory drugs). If they experience moderate cervical spondylosis, they may need a prescription-strength NSAID.
Other common treatments include the following.
- Applying heat or ice
- Walking
- Taking medications – muscle relaxants, corticosteroids, antidepressants or anti-seizure medications
- Steroid-based injections for pain relief
- Physical therapy
- Surgery as a last result to relieve nerve pressure in the spinal canal
FAQ
How to Prevent Cervical Spondylosis?
The cervical spondylosis that is a result of a normal aging process cannot be prevented. However, you can slow down its onset and control the severity of symptoms. For example, learning to lift objects correctly, wearing appropriate protective gear during athletic activities and maintaining good posture at all times can help maintain a healthy spine from neck to lower back. Other preventive measures include getting regular exercise to maintain strong muscles and ligaments, maintaining healthy body weight, following a nutrient-rich diet and not smoking.
When Should You See a Pain Management Doctor?
You should see a pain management doctor when:
- pain is persistent for more than 2-3 weeks
- pain interferes with daily activities
- pain continues to increase in severity despite home remedies.
- pain radiates beyond the neck into the arm or leg
- you have any doubts about the cause of pain, no matter how long it has endured
- pain in your neck began after an injury or fall
What is the Difference Between Cervical Spondylosis and Spinal Osteoarthritis?
Cervical spondylosis is a catch-all term that refers to changes occurring in the discs, joints, and bones located in the neck. It is also referred to as cervical osteoarthritis. The osteoarthritis develops as a result of aging, injury, or disease.
The spine has three major segments – cervical (neck), thoracic (mid-back), and lumbar (lower back). Spinal osteoarthritis refers to osteoarthritis occurring anywhere along the spine. No matter where osteoarthritis occurs, the condition can cause inflammation of the spinal facet joints, bone spurs, and pain.
What is the Best Treatment for Cervical Spondylosis?
The best home treatments for cervical spondylosis are applying ice and heat, gentle exercises that stretch neck muscles and ligaments and taking over-the-counter anti-inflammatory medications.
The best treatment beyond home care usually begins with prescription anti-inflammatory medications and physical therapy, including specific stretches and exercises to strengthen muscles and ligaments to relieve pain. If these approaches do not help the pain, the doctor may suggest steroid injections.