The two most common types of arthritis are rheumatoid arthritis and osteoarthritis. Both affect joints, and both can be painful and debilitating. However, they are different in terms of their underlying cause and the full range of physical impacts.
Rheumatoid Arthritis vs Osteoarthritis: What is common
Rheumatoid arthritis and osteoarthritis have some things in common. The most obvious commonality is that both affect joints. There is no doubt that both can significantly harm the quality of life, if the disease is not purposefully managed. The most significant difference between the two types of arthritis is the underlying cause.
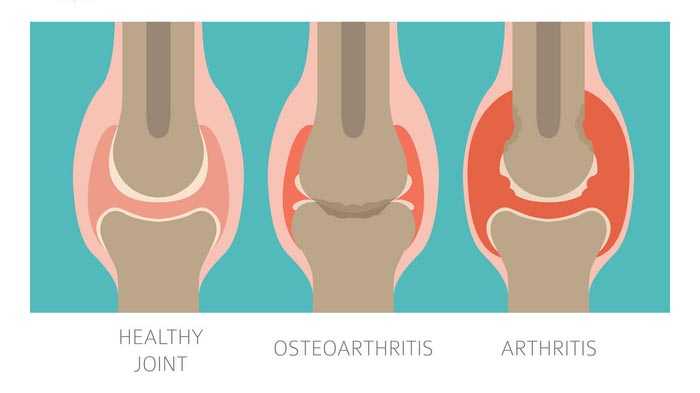
The most familiar type of arthritis is osteoarthritis OA, also called the wear-and-tear disease. Arthritis a degenerative disease develops when the cushioning cartilage in the joint wears out or disintegrates. Pain occurs when bones rub against each other. Sometimes, bone spurs develop, increasing pain and causing inflammation in surrounding tissues.
Another common occurrence is when bits of bone or cartilage float around in the joint, causing painful inflammation. Osteoarthritis will continue to get worse over time, which is why it is called degenerative. Eventually, all the cartilage wears away.
Rheumatoid Arthritis vs Osteoarthritis: Causes
The cause of rheumatoid arthritis is quite different and still not fully understand. Rheumatoid arthritis is an inflammatory autoimmune disease. A properly functioning immune system attacks foreign substances. In the case of an autoimmune disease, the immune system attacks healthy tissues instead, as if they are foreign substances.
In rheumatoid arthritis what is happening? In this situation, the immune system attacks joints and other tissues and systems, and the result is inflammation of the synovium or joint lining. Synovial inflammation is regulated by cytokines. In rheumatoid arthritis, pro-inflammatory cytokines are present in such a large number that they promote inflammatory responses and induce cartilage degradation. The synovium produces the lubrication fluid for the joint. An inflamed synovium thickens, causing swelling in the joint, which can produce severe pain.
Osteoarthritis is contained in the affected joint and nearby tissues. The inflammatory reaction associated with rheumatoid arthritis is not necessarily contained in joints. It can damage other parts of the body, like organ linings, blood vessels, and eyes.
Osteoarthritis vs Rheumatoid Arthritis: Symptoms
Osteoarthritis and rheumatoid arthritis share some similar symptoms, but there are also a number of differences. Symptoms common to both include joint:
- Pain
- Tenderness
- Swelling
- Stiffness, especially in the morning
- Warmth
- Deformity over time
- Restricted range of motion
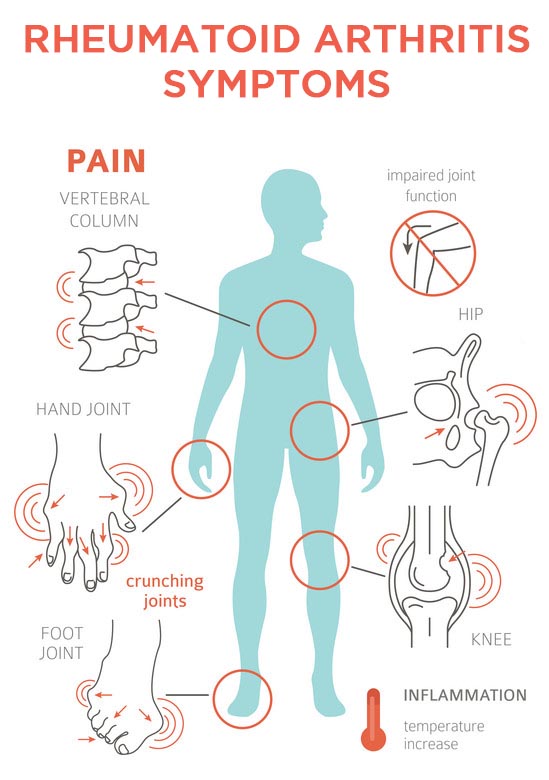
Pain is listed first because in evaluating osteoarthritis vs rheumatoid arthritis pain, a person experiencing either disease will have similar joint pain. Osteoarthritis pain will develop slowly because the disease progresses slowly. Rheumatoid arthritis pain can worsen within weeks or months, so pain is felt earlier.
Another one of the main differences between the two diseases is that rheumatoid arthritis is more widespread, so it can cause havoc throughout the body. Some symptoms beyond the ones mentioned earlier include:
- Fatigue
- General malaise or depression
- Low-grade fever
- Symmetrical joint swelling
- Synovial cysts
- Rheumatoid nodules
- Displaced or ruptured tendons
- Restricted lung functioning
- Atherosclerosis
- Eye disease
- Sjogren’s Syndrome (affects lacrimal and salivary glands)
- Rheumatoid vasculitis
- Peripheral neuropathy
Left untreated, rheumatoid arthritis can develop symptoms that are actually additional diseases.
Differences between RA and OA
As rheumatoid arthritis progresses, the more severe symptoms appear. Following are some differences between rheumatoid arthritis and osteoarthritis.
- RA is an autoimmune disease so the immune system is compromised, but in osteoarthritis autoimmune issues are not present.
- RA symptoms have a rapid onset, while OA progresses slowly.
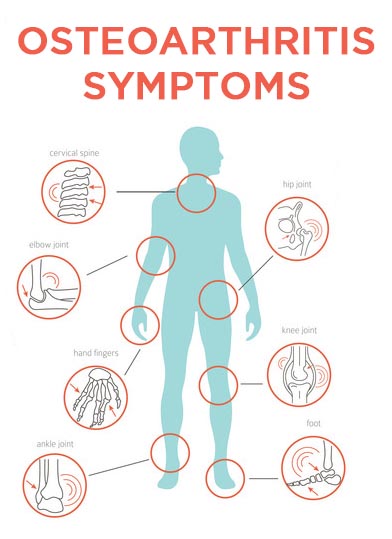
- RA affects joints throughout the body, while OA affects mostly knees, small finger joints, thumb and hips (though OA can impact any joint, including in the spine).
- RA creates systemic symptoms, like fatigue and low-grade fever, while OA is localized to a joint.
- RA is symmetrical, so both sides of the body are affected in similar joints, while OA affects individual joints.
- RA morning stiffness may last longer than 30 minutes, while the stiffness people with OA experiences is likely to ease within 30 minutes.
Osteoarthritis vs Rheumatoid Arthritis Diagnosis
Rheumatoid arthritis is diagnosed by performing several tests. There is no single test that identifies rheumatoid arthritis:
- Physical examination to look for swelling, redness and other outward physical symptoms.
- Blood tests look for the rheumatoid factor, anti-CCP and antinuclear antibodies, and the level of inflammation.
- Imaging tests that include x-rays, MRIs and/or ultrasounds.
Considering what can be determined by an osteoarthritis vs rheumatoid arthritis xray, the x-ray is more beneficial for detecting osteoarthritis because the disease involves the bones in its early stages. Rheumatoid arthritis may not present itself in the bones in its early stages. Instead, the patient may experience non-bone issues first, like chronic fatigue, or synovial and tendon inflammation. For this reason, the MRI and ultrasound are better than x-rays for early diagnose of rheumatoid arthritis.
Which Arthritis is worse?
A common question people ask goes like this: Is osteoarthritis worse than rheumatoid arthritis? Rheumatoid arthritis is a more complex and widespread disease. It presents itself differently in each patient and is more difficult to diagnose because of its complexity. It can lead to other diseases, like cardiopulmonary disease and makes people more susceptible to diseases like lupus.
Osteoarthritis is localized in the joint, and some joints can be replaced if the damage from arthritis is severe. It does not impact organs or lead to other diseases.
However, both diseases are chronic and neither is curable. They both affect the quality of life. It is important to address the symptoms as soon as they appear. In both types of arthritis, the sooner treatment begins, the better.
